***** Much like most blogs, this blog contains affiliate links. I do not mention products that I don’t personally consume (or give to my family). For more information, please visit my Privacy Policy page. Thanks for reading *****
February 2019
Do you have any idea how hard it is to knowingly give something to your child, when you know that it is hurting him? This is how I feel about gluten. It goes against every fiber in my body to feed it to my oldest child. While he’s not been officially diagnosed with Celiac, my husband and I are both certain that his body hates gluten.
This week, we are finally going in for my Gluten Free Kid’s (GFK) endoscopy to find out one way or another if he has Celiac Disease. I say finally, because it has taken us two years to get to this point. He’s been in and out of doctors’ offices; he’s had tons of blood tests, swab tests, xRays, etc., and now we’re gearing up for a 2-hour trip to get his endoscopy done this week.
You may be wondering why it takes so long to get a diagnosis. Why is there the need for so many tests? Well, believe it or not, it is extremely difficult diagnose Celiac Disease. There are many factors that need to add up in order for a gastroenterologist (GI) to diagnosis someone with the disease. If you are interested in learning more about the facts of Celiac Disease, check out this Celiac Disease Facts and Figures document from the Celiac Disease Center from the University of Chicago Medical Center.
My kiddo has been through so many tests, and in many ways, it is a relief to know that he (we) will finally have something concrete to pin all of his symptoms on. In other ways, getting the procedure done is a bit unsettling. Any time your child is put under anesthesia, there is the potential for something to go awry. Everyone has told us that it is an easy procedure, but I’m a mom people. It’s my job to worry.
Whatever happens on Wednesday, he will once again be gluten free on Thursday. We all know (including him, us and his GI doctor) that he is much healthier when he doesn’t eat gluten, so back to a GF household we go.
Yes, I say back to a GF household. A little over two years ago, we started our gluten-free adventure. However, my son has been reacting to gluten since he was an infant, we just didn’t know it then. Here’s what his gluten reactions looked like as a infant and toddler…
My Sick Baby
So my GFK was a generally happy baby, BUT he was sick. All. The. Time. Thank God he didn’t have colic too, because I’m not sure how I would’ve lived through that. We were in and out of the doctor’s office several times a year getting prescription after prescription of antibiotics, steroids, creams, ointments, and sprays. You name it, he was on it to combat his symptoms.

His list of symptoms included constant congestion, runny nose, puffiness, rashes, and itchiness. He had his tonsils and adenoids removed, when he was four to try to alleviate some of the symptoms. He had allergies. Clearly, he had seasonal allergies, but he was also reacting to something in the environment.
So, naturally, I started cleaning everything. He slept hiked up on pillows, so he could breathe at night, and I always had a humidifier running. He was on allergy meds year round (he takes Children’s Zyrtec). Then in the spring and summer when his seasonal allergies really kicked in, he was also taking Benedryl several times a week to combat clear allergic reactions. During those times, he was also taking a daily dose of a nasal spray (prescription) and eye drops as needed. Ugh, my perfect little kiddo was struggling with something, and I couldn’t figure it out
Symptoms in School
As he started to play sports and go to school, I noticed that these symptoms were slowing him down. When he was in kindergarten, I found him scratching the palms of his hands like crazy. Again, we went to the doctors for a steroid to kick the symptoms out of him. I finally asked them, when do we start looking into what is causing his symptoms rather than just treating them. (Pandora’s box officially opened right then.)
That moment started our journey from the pediatrician’s office, to the allergist’s office, then onto the two different pediatric gastroenterologists’s offices. At first, I was certain that he was allergic to something, I just didn’t know what it was. I was relatively certain it was something in the environment, like a perfume or other chemical. It hadn’t yet occurred to me that it might be something he was ingesting.
Bye, Bye Chemicals
We tried eliminating as many chemicals from our house as we could. Goodbye candles, harsh detergents, air fresheners, and the like. I stopped using chemicals to clean and instead moved to using white vinegar and Norex products. For his personal cleansing products we exclusively used the California Baby Super Sensitive Products.
So did it work, getting rid of the chemicals? Umm, it helped, but it didn’t work. I was able to calm his symptoms faster using more natural and safer products, but he still had all of his symptoms. So, we managed them. (Six years ago, I wrote this post about his Eczema. (We have since moved away from Tide -> Check out My Green Fills, you can get 50 Loads FREE Here. It smells great; the company is eco- and socially- responsible; and it works for all of the laundry in our home.)
What is Celiac Disease?
In the midst of trying to see what my child was reacting to, some surprising information came our way. My husband’s brother was diagnosed with Celiac’s Disease. So, naturally, our family was chatting quite a bit about what Celiac Disease is and how his diagnosis was going to affect future family meals, holidays, etc. Truthfully, he was quite startled by the diagnosis too, because he didn’t have any symptoms. (Well, not any intestinal discomfort or things you would naturally assume Celiac Disease would cause.) He had been going back and forth to the doctor because his blood work kept coming back strange. His thyroid numbers, cholesterol, and liver enzymes were all wonky.
Shortly after these discussions started, my kiddo went in for his annual checkup. For this appointment, the doctor ran a blood panel, which was the first one that he had received. When we went in for his appointment, all looked OK, but my son’s cholesterol was elevated. What? I know I haven’t mentioned this before, but we’re talking about a kid who LOVES steamed rice, chicken, and broccoli. He is not and was not on a steady diet of deep-fried food. Both my husband and I were stunned by this information; it just didn’t seem right.
In the spring of 2016, I saw this post. It was so simple, but it was something I hadn’t considered before. According to the article, “Can Allergies Be Causing Your Baby’s Sniffles?” from the Burdett Birth Center,
“Even though pollen counts are high, and the breezy spring days have you sneezing, it’s unlikely your infant is suffering from seasonal allergies. According to physicians, allergies develop only after cumulative exposure to allergens. Your infant would need to have significant exposure to something like tree pollen, grass or ragweed to trigger a seasonal allergy, and most infants simply don’t spend that much time outdoors in their first year of life to make that happen.
While you can probably rule out seasonal allergies as the culprit for your little one’s symptoms, you can’t rule out allergies altogether. In fact, the CDC reports that allergic reactions to food and indoor elements are on the rise in children.”
https://www.burdettbirthcenter.org/blog/caring-for-newborns/can-seasonal-allergies-be-causing-your-babys-sniffles/
Wait, what?!? It was unlikely that my baby had had seasonal allergies? Then what the heck were we treating with all of those antihistamines for all of those years? Is there something more here? Was I inadvertently giving him something to eat that he was allergic to?
So, Gluten Showed Up Too!
In the summer of 2016, I ran across an offer for an allergy and intolerance test that I could perform at home and then send away for the results. I just sent a lock of his hair to the group. Then, two lists came back from that test. The first was a list of deficiencies that he had, and the second was a list of intolerances that he could potentially have. So, we were not surprised to see ragweed on the list, as well tree allergies. However, lo and behold, gluten showed up too!
At this point, I had so many questions. Could gluten really be at the bottom of all of his symptoms? So, grrl, you know what I did. That’s right, I Google’d my heart out; I started asking questions; and I began watching my boy like a hawk. Yes, of course, my family and friends thought that I was crazy. That’s not news though, I’ve always been a bit on the wacky side.
It was a huge leap for the people close to us to see a connection from my son’s symptoms to any type of gluten issue. Plus something new started to emerge, my GFK started to react emotionally to the foods he was ingesting. Have you heard of people reacting to food colorings and additives? Well, for a few years, there were several families locally speaking publicly about this. The way that these parents were explaining how their kids were reacting to the dyes in food were very similar to the way that my son was reacting to food in general.
Symptoms After Eating
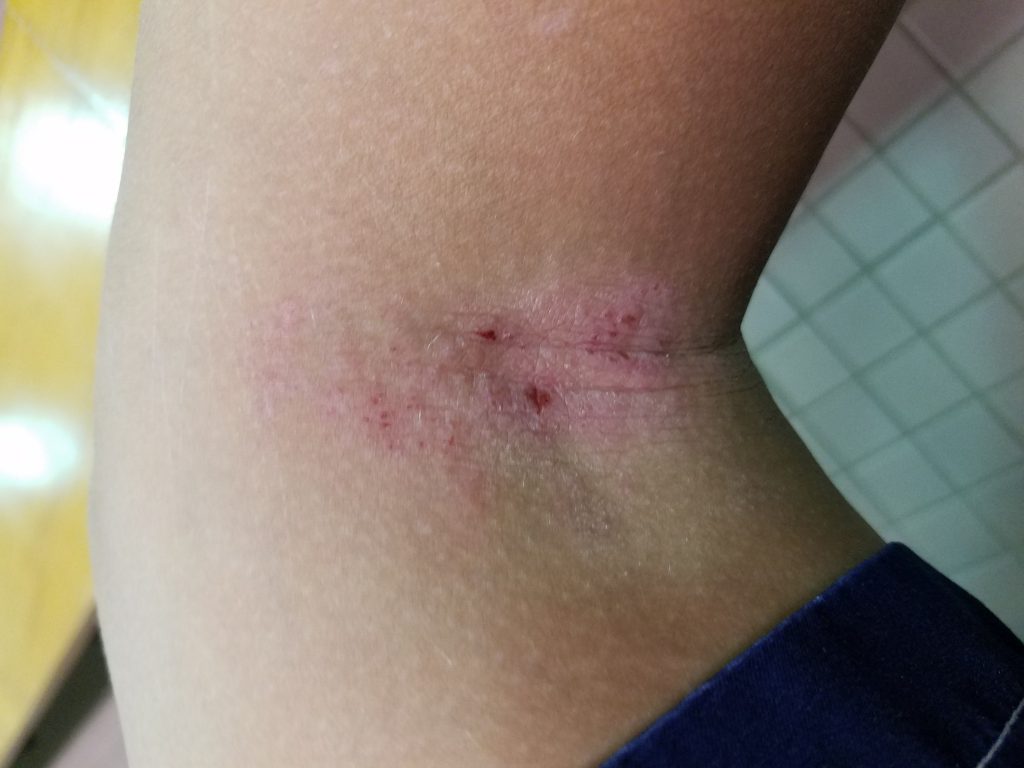
For several months, I just watched him and cataloged the way he responded to food. It quickly became apparent to me that he was, in fact, reacting to gluten. After meals, he would get bloated, he was on the toilet constantly, his rashes continued (the worst rash appeared behind his knees and in his elbow crevices), and shortly after he ate he turned into the incredible hulk. He would become frantic, sad, and angry. It was like my 8 year old had teenage angst.
Frankly, my husband thought I was nuts. He said, “he’s just emotional, he’s being bad, he’s too sensitive, etc.” And then it happened. We were in the perfect situation, where I could predict his reaction right before my husband’s eyes.
We had taken a family day trip to Niagara Falls, and everyone’s spirits were elevated. We were all smiles and giggles, and we stopped to have a bite to eat. My son had not had anything that contained gluten all day, and then he asked for pizza for lunch. My husband says, “sure,” and I’m delighted, because I know exactly what’s about to happen. The light-hearted chatter continued, and I leaned over to my husband, while my boys were busy playing a game together and I said, “Just watch. He’s fine now, right? Watch what happens after the pizza.” My husband agreed to play along and watch my son as he ate.
Sure enough, within minutes of eating the pizza, he was crying at the table. What’s worse was that he couldn’t articulate why he was crying. When we asked him, he said, “I don’t know, I just don’t know!” While there was nothing amusing about the situation, because it was awful to see him helpless, it was wonderful that my husband finally saw it with his own eyes. My husband saw that maybe there was something more to this gluten thing than he originally thought.
With my husband as part of the watch team, he was able to see my son continue to display clear emotional symptoms within minutes of eating gluten. He also noticed the bloating, the rashes getting worse, and his loss of healthy coloring in his face. My GFK had dark circles under his eyes and an ashiness that didn’t not look right.

Doctors, Doctors, and More Doctors
By this time, the allergist couldn’t confirm or deny a gluten issue, because if it was Celiac, it wouldn’t be an allergy. Then they didn’t want to do a panel on him, because they thought he was too young to proceed with that type of testing, since no reactions so far seemed life threatening. I know, you can imagine how deflating that is to hear as a mom.
Next, we moved on to the first pediatric gastroenterologist. AND we had taken my son off of gluten. At that point, it was clear as day to us that he was reacting to gluten, and I couldn’t bear to keep him on something I knew his body was rejecting. We saw the first GI doctor several times. He did have the Celiac gene, and I laid out all of his symptoms. I was dismissed and asked if I had considered counseling for my son. (Umm, counseling? Listen, I’m not opposed to counseling, I have seen a counselor a couple of times when I was working through some bereavement issues. But, what would my son need a counselor for here? That really struck a “hey, crazy mom, you have no idea what your son has or needs” nerve.”) It wasn’t until I mentioned the family history of my brother-in-law’s Celiac diagnosis and my mother-in-law’s Colitis diagnosis that he started to really listen to me. The next step there was to schedule an endoscopy, but I left that appointment both disappointment and upset with the whole process.
Granted, healthcare professionals should absolutely rely on real data to diagnose conditions, but to so flippantly disregard the information I was bringing to the table made me realize that wasn’t the doctor my son needed.
We’re Done With Doctors
So, we walked away from doctors for close to two years. Obviously, we still saw his pediatrician, who understood our situation. He continued to emphasized the importance of a GF diet to our kiddo, even though we never received the formal diagnosis. However, we were done with specialists.
Ahhh! He Feels Better!
Over the course of time, he stopped taking every one of his medications and has moved to an only as needed status. So for two weeks in the spring, when the trees are in bloom, he will take his allergy medication. That’s it. It’s absolutely amazing and such a relief. Even my eleven year old can see the change within himself. He has no interest in eating gluten, because he understands how much better he feel off of it.
For such a long stretch, this was our normal, and it was just fine for us. Of course, this article started with the anxieties of a mother bringing her child in for an endoscopy, so how do you do that without a doctor’s orders? Well, you don’t.
Do We Need a Diagnosis?
Next year, my GFK starts middle school, and it will be difficult to get him out of class for long stretches of time. And that is only going to get worse as he gets older, so we had to consider that it’s now or never. By some stroke of luck, I overheard a friend talking about her experience with a pediatric gastroenterologist who she respected. He wasn’t a doctor I had heard of before and he was two hours away.
Well, we took a shot on him, and he turned out to be fantastic. He listened to me, asked questions, AND explored the family history. Plus, he spoke with my son extensively. He eased his concerns, and he made him laugh. So here we are, after numerous blood tests, an upper GI with a follow through, prepping for an endoscopy.
In order to prep for all of the tests he took this year, we had to put gluten back into his diet. So, every day, our son had a small serving of food with gluten in it. Guess what? His symptoms returned. His rashes, his congestion, his mood swings, his tummy issues and bloating. All of the symptoms returned, so we knew without a doubt that our child has some significant gluten issues.
Now, to find out if he has Celiac Disease…
—-
March 2019
So, he did it. He made it through his endoscopy. He was a champ and the procedure took about a half hour. We’re home before school let out for the day. We had to wait a couple of weeks for the results. Here’s what we found out…
The test results were inconclusive enough for the GI doctor to hold off on the Celiac diagnosis, rather he’s treating him for Non-Celiac Gluten Sensitivity. Some of his blood tests indicated Celiac, while others were normal. The his intestines looked good, but a couple of the biopsies came back indicating inflammation.
With the family history, and the fact that my son was off of gluten for so long before he had the endoscopy, the doctor admitted that the diagnosis could’ve swung to early stage Celiac. The doctor explained that in the future there will be different types of Celiac to help zero in on some of the symptoms and causes. So some people will have something like Celiac Type A, while others have Celiac Type B.
If he were to diagnosis my kiddo with Celiac, he would be obliged to follow up with him at regular intervals, to give him tests and to follow the progression of the disease. With the Non-Celiac Gluten Sensitivity diagnosis, my son still needs to follow a gluten free diet, but we can follow up with the doctor if/when we notice any symptom changes. As a rule, we would rather try to combat something through diet and exercise, if it is possible, so this seems like the perfect outcome for us. No one wants to have their kid spending too much time in a doctor’s office, especially if we can manage his symptoms at home.
So here we are, years after we started this journey, and it looks like by some amazing stroke of fate (and a bit of luck), we were able to determine that my son reacts to gluten. We hope that he never develops Celiac Disease and that now he’s in a better place to ward off the other autoimmune conditions and concerns that come with it.
However, in the meantime, my husband has now started his Celiac inquiry, because his recent blood work came back wonky. It looks like his doctors are faster to diagnose him than our son.
As far as I’m concerned, I’d rather my son not have Celiac Disease, so I’d say his endoscopy was a success. Who knows, perhaps those couple of years off of gluten gave his system enough time to heal, so he didn’t actually develop it. There is so much research that still needs to be done in order to get a clear understanding of these murky conditions. While it is nice to be able to definitively say this is the problem, I’m much happier in limbo knowing my son is feeling better and growing well.
Now, onto the next kiddo. His struggle went from a slow bowel as a toddler to a constantly loose bowel as an elementary school student. Anyone else thinking, what I’m thinking? Here we go again…
—
How’s your kiddo doing? Does he or she have any similar experiences to my GFK? Please share your stories in the comments below.
